Research Report Series: Cocaine Abuse and Addiction
Download PDF Version What is PDF?
Source: NIDA Research Report Series: Cocaine Abuse and Addiction, NIH
Publication Number 99-4342, May, 1999,
Revised November 2004
Public Domain
Table of Contents (TOC)
From the DirectorChapter 1: What is cocaine?
Chapter 2: What is crack?
Chapter 3: What is the scope of cocaine use in the United States?
Chapter 4: How is cocaine used?
Chapter 5: How does cocaine produce its effects?
Chapter 6: What are the short-term effects of cocaine use?
Chapter 7: What are the long-term effects of cocaine use?
Chapter 8: What are the medical complications of cocaine abuse?
Chapter 9: Are cocaine abusers at risk for contracting HIV/AIDS and hepatitis B and C?
Chapter 10: What is the effect of maternal cocaine use?
Chapter 11: What treatments are effective for cocaine abusers?
Glossary
References
Cocaine abuse and addiction continues to be a problem that plagues our nation. For instance, from 1965 to 1967, only 0.1 percent of youths had ever used cocaine, but rates rose throughout the 1970s and 1980s, reaching 2.2 percent in 1987. After a brief decline, lifetime prevalence rates peaked at 2.7 percent in 2002.
 However, we now know more about where and how cocaine acts in the brain,
including how the drug produces its pleasurable effects and why it is
so addictive. Through the use of sophisticated technology, scientists
can actually see the dynamic changes that occur in the brain as an individual
takes the drug. They can observe the different brain changes that occur
as a person experiences the “rush,” the “high,” and,
finally, the craving of cocaine. They can also identify parts of the
brain that become active when a cocaine addict sees or hears environmental
stimuli that trigger the craving for cocaine. Because these types of
studies pinpoint specific brain regions, they are critical to identifying
targets for developing medications to treat cocaine addiction.
However, we now know more about where and how cocaine acts in the brain,
including how the drug produces its pleasurable effects and why it is
so addictive. Through the use of sophisticated technology, scientists
can actually see the dynamic changes that occur in the brain as an individual
takes the drug. They can observe the different brain changes that occur
as a person experiences the “rush,” the “high,” and,
finally, the craving of cocaine. They can also identify parts of the
brain that become active when a cocaine addict sees or hears environmental
stimuli that trigger the craving for cocaine. Because these types of
studies pinpoint specific brain regions, they are critical to identifying
targets for developing medications to treat cocaine addiction.
One of NIDA’s most important goals is to translate what scientists learn from research, in order to help the public better understand drug abuse and addiction, and to develop more effective strategies for their prevention and treatment. We hope that this compilation of scientific information on cocaine will help to inform readers about the harmful effects of cocaine abuse, and that it will assist in prevention and treatment efforts.
Nora D. Volkow, M.D.
Director
National Institute on Drug Abuse
 Cocaine
is a powerfully addictive stimulant that directly affects
the brain. Cocaine was labeled the drug of the 1980s and ‘90s,
because of its extensive popularity and use during this
period. However, cocaine is not a new drug. In fact, it
is one of the oldest known drugs. The pure chemical, cocaine
hydrochloride, has been an abused substance for more than
100 years, and coca leaves, the source of cocaine, have
been ingested for thousands of years.
Cocaine
is a powerfully addictive stimulant that directly affects
the brain. Cocaine was labeled the drug of the 1980s and ‘90s,
because of its extensive popularity and use during this
period. However, cocaine is not a new drug. In fact, it
is one of the oldest known drugs. The pure chemical, cocaine
hydrochloride, has been an abused substance for more than
100 years, and coca leaves, the source of cocaine, have
been ingested for thousands of years.
Pure cocaine was first extracted from the leaf of the Erythroxylon coca bush, which grows primarily in Peru and Bolivia, in the mid-19th century. In the early 1900s, it became the main stimulant drug used in most of the tonics/elixirs that were developed to treat a wide variety of illnesses. Today, cocaine is a Schedule II drug, meaning that it has high potential for abuse, but can be administered by a doctor for legitimate medical uses, such as local anesthesia for some eye, ear, and throat surgeries.
There are basically two chemical forms of cocaine: the hydrochloride salt and the “freebase.” The hydrochloride salt, or powdered form of cocaine, dissolves in water and, when abused, can be taken intravenously (by vein) or intranasally (in the nose). Freebase refers to a compound that has not been neutralized by an acid to make the hydrochloride salt. The freebase form of cocaine is smokable.
Cocaine is generally sold on the street as a fine, white, crystalline powder, known as “coke,” “C,” “snow,” “flake,” or “blow.” Street dealers generally dilute it with such inert substances as cornstarch, talcum powder, and/or sugar, or with such active drugs as procaine (a chemically related local anesthetic) or with such other stimulants as amphetamines.
Crack is the street name given to a freebase form of cocaine that has been processed from the powdered cocaine hydrochloride form to a smokable substance. The term “crack” refers to the crackling sound heard when the mixture is smoked. Crack cocaine is processed with ammonia or sodium bicarbonate (baking soda) and water, and heated to remove the hydrochloride.
Because crack is smoked, the user experiences a high in less than 10 seconds. This rather immediate and euphoric effect is one of the reasons that crack became enormously popular in the mid 1980s. Another reason is that crack is inexpensive both to produce and to buy. Crack cocaine remains a serious problem in the United States. The National Survey on Drug Use and Health (NSDUH) estimated the number of current crack users to be about 567,000 in 2002.
In 2002, an estimated 1.5 million Americans could be classified as dependent on or abusing cocaine in the past 12 months, according to the NSDUH. The same survey estimates that there are 2.0 million current (past-month) users. Cocaine initiation steadily increased during the 1990s, reaching 1.2 million in 2001.
Adults 18 to 25 years old have a higher rate of current cocaine use
than those in any other age group. Overall, men have a higher rate of
current cocaine use than do women. Also, according to the 2002 NSDUH,
estimated rates of current cocaine users were 2.0 percent for American
Indians or Alaskan Natives, 1.6 percent for African-Americans, 0.8 percent
for both Whites and Hispanics, 0.6 percent for Native Hawaiian or other
Pacific Islanders, and
0.2 percent for Asians.
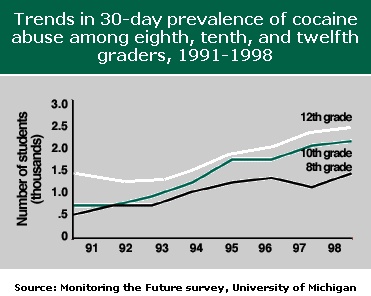
The 2003 Monitoring the Future Survey, which annually surveys teen attitudes and recent drug use, reports that crack cocaine use decreased among 10th-graders in 30-day, annual, and lifetime use prevalence periods. This was the only statistically significant change affecting cocaine in any form. Past-year use of crack declined from 2.3 percent in 2002 to 1.6 percent in 2003. Last year, the rate increased from 1.8 percent to 2.3 percent, and this year’s decline brings it to approximately its 2001 level.
Data from the Drug Abuse Warning Network (DAWN) showed that cocaine-related emergency department visits increased 33 percent between 1995 and 2002, rising from 58 to 78 mentions per 100,000 population.
The principal routes of cocaine administration are oral, intranasal, intravenous, and inhalation. The slang terms for these routes are, respectively, “chewing,” “snorting,” “mainlining” or “injecting,” and “smoking” (including freebase and crack cocaine). Snorting is the process of inhaling cocaine powder through the nostrils, where it is absorbed into the bloodstream through the nasal tissues. Injecting releases the drug directly into the bloodstream, and heightens the intensity of its effects. Smoking involves the inhalation of cocaine vapor or smoke into the lungs, where absorption into the bloodstream is as rapid as by injection. The drug also can be rubbed onto mucous tissues. Some users combine cocaine powder or crack with heroin in a “speedball.”
Cocaine use ranges from occasional use to repeated or compulsive use, with a variety of patterns between these extremes. Other than medical uses, there is no safe way to use cocaine. Any route of administration can lead to absorption of toxic amounts of cocaine, leading to acute cardiovascular or cerebrovascular emergencies that could result in sudden death. Repeated cocaine use by any route of administration can produce addiction and other adverse health consequences.
A great amount of research has been devoted to understanding the way cocaine produces its pleasurable effects, and the reasons it is so addictive. One mechanism is through its effects on structures deep in the brain. Scientists have discovered regions within the brain that are stimulated by rewards. One neural system that appears to be most affected by cocaine originates in a region located deep within the brain called the ventral tegmental area (VTA). Nerve cells originating in the VTA extend to the region of the brain known as the nucleus accumbens, one of the brain’s key areas involved in reward. In studies using animals, for example, all types of rewarding stimuli, such as food, water, sex, and many drugs of abuse, cause increased activity in the nucleus accumbens.

Researchers have discovered that, when a rewarding event is occurring, it is accompanied by a large increase in the amounts of dopamine released in the nucleus accumbens by neurons originating in the VTA. In the normal communication process, dopamine is released by a neuron into the synapse (the small gap between two neurons), where it binds with specialized proteins (called dopamine receptors) on the neighboring neuron, thereby sending a signal to that neuron. Drugs of abuse are able to interfere with this normal communication process. For example, scientists have discovered that cocaine blocks the removal of dopamine from the synapse, resulting in an accumulation of dopamine. This buildup of dopamine causes continuous stimulation of receiving neurons, which is associated with the euphoria commonly reported by cocaine abusers.
As cocaine abuse continues, tolerance often develops. This means that higher doses and more frequent use of cocaine are required for the brain to register the same level of pleasure experienced during initial use. Recent studies have shown that, during periods of abstinence from cocaine use, the memory of the euphoria associated with cocaine use, or mere exposure to cues associated with drug use, can trigger tremendous craving and relapse to drug use, even after long periods of abstinence.

Cocaine’s effects appear almost immediately after a single dose, and disappear within a few minutes or hours. Taken in small amounts (up to 100 mg), cocaine usually makes the user feel euphoric, energetic, talkative, and mentally alert, especially to the sensations of sight, sound, and touch. It can also temporarily decrease the need for food and sleep. Some users find that the drug helps them perform simple physical and intellectual tasks more quickly, while others experience the opposite effect.
The duration of cocaine’s immediate euphoric effects depends upon the route of administration. The faster the absorption, the more intense the high. Also, the faster the absorption, the shorter the duration of action. The high from snorting is relatively slow in onset, and may last 15 to 30 minutes, while that from smoking may last 5 to 10 minutes.
The short-term physiological effects of cocaine include constricted blood vessels; dilated pupils; and increased temperature, heart rate, and blood pressure. Large amounts (several hundred milligrams or more) intensify the user’s high, but may also lead to bizarre, erratic, and violent behavior. These users may experience tremors, vertigo, muscle twitches, paranoia, or, with repeated doses, a toxic reaction closely resembling amphetamine poisoning. Some users of cocaine report feelings of restlessness, irritability, and anxiety. In rare instances, sudden death can occur on the first use of cocaine or unexpectedly thereafter. Cocaine-related deaths are often a result of cardiac arrest or seizures followed by respiratory arrest.

Cocaine is a powerfully addictive drug. Thus, an individual may have difficulty predicting or controlling the extent to which he or she will continue to want or use the drug. Cocaine’s stimulant and addictive effects are thought to be primarily a result of its ability to inhibit the reabsorption of dopamine by nerve cells. Dopamine is released as part of the brain’s reward system, and is either directly or indirectly involved in the addictive properties of every major drug of abuse.
An appreciable tolerance to cocaine’s high may develop, with many addicts reporting that they seek but fail to achieve as much pleasure as they did from their first experience. Some users will frequently increase their doses to intensify and prolong the euphoric effects. While tolerance to the high can occur, users can also become more sensitive (sensitization) to cocaine’s anesthetic and convulsant effects, without increasing the dose taken. This increased sensitivity may explain some deaths occurring after apparently low doses of cocaine.
Use of cocaine in a binge, during which the drug is taken repeatedly and at increasingly high doses, leads to a state of increasing irritability, restlessness, and paranoia. This may result in a full-blown paranoid psychosis, in which the individual loses touch with reality and experiences auditory hallucinations.

There can be severe medical complications associated with cocaine use. Some of the most frequent complications are cardiovascular effects, including disturbances in heart rhythm and heart attacks; respiratory effects such as chest pain and respiratory failure; neurological effects, including strokes, seizures, and headaches; and gastrointestinal complications, including abdominal pain and nausea.
Cocaine use has been linked to many types of heart disease. Cocaine has been found to trigger chaotic heart rhythms, called ventricular fibrillation; accelerate heartbeat and breathing; and increase blood pressure and body temperature. Physical symptoms may include chest pain, nausea, blurred vision, fever, muscle spasms, convulsions, coma, and death.
Different routes of cocaine administration can produce
different adverse effects. Regularly snorting cocaine,
for example, can lead to loss of sense of smell,
nosebleeds, problems with swallowing, hoarseness,
and an overall irritation of the nasal septum, which
can lead to a chronically inflamed, runny nose. Ingested
cocaine can cause severe bowel gangrene, due
to reduced blood flow. And, persons who inject cocaine have puncture marks
and “tracks,” most commonly in their forearms. Intravenous cocaine
users may also experience an allergic reaction, either to the drug, or to some
additive in street cocaine, which can result, in severe cases, in death. Because
cocaine has a tendency to decrease food intake, many chronic cocaine users
lose their appetites and can experience significant weight loss and malnourishment.
Research has revealed a potentially dangerous interaction between cocaine and alcohol. Taken in combination, the two drugs are converted by the body to cocaethylene. Cocaethylene has a longer duration of action in the brain and is more toxic than either drug alone. While more research needs to be done, it is noteworthy that the mixture of cocaine and alcohol is the most common two-drug combination that results in drug-related death.
Yes. Cocaine abusers, especially those who inject, are at increased risk for contracting such infectious diseases as human immunodeficiency virus (HIV/AIDS) and viral hepatitis. In fact, use and abuse of illicit drugs, including crack cocaine, are major risk factors for new cases of HIV. Drug abuse-related spread of HIV can result from direct transmission of the virus through the sharing of contaminated needles and paraphernalia between injecting drug users. It can also result from indirect transmission, such as an HIV-infected mother transmitting the virus perinatally to her child. This is particularly alarming given that 30 percent of all new AIDS cases are among women. Research has also shown that drug use can interfere with judge- ment about risk-taking behavior, and can potentially lead to reduced precautions regarding sexual behaviors, the sharing of needles and injection paraphernalia, and the trading of sex for drugs, by both men and women.
Additionally, hepatitis C (HCV) has spread rapidly among injection drug users; Centers for Disease Control and Prevention (CDC) estimates indicate infection rates of 50 to 80 percent in this population. While currently available treatment is not effective for everyone and can have significant side effects, medical followup is essential for all those who are infected. At present, there is no vaccine for the hepatitis C virus. The virus is highly transmissible via injection, and HCV testing is recommended for any individual who has ever injected drugs.
 The full extent of the effects of prenatal drug
exposure on a child is not completely known, but
many scientific studies have documented that babies
born to mothers who abuse cocaine during pregnancy
are often prematurely delivered, have low birth weights
and smaller head circumferences, and are often shorter
in length.
The full extent of the effects of prenatal drug
exposure on a child is not completely known, but
many scientific studies have documented that babies
born to mothers who abuse cocaine during pregnancy
are often prematurely delivered, have low birth weights
and smaller head circumferences, and are often shorter
in length.
Estimating the full extent of the consequences of maternal drug abuse is difficult, and determining the specific hazard of a particular drug to the unborn child is problematic for many reasons. Multiple factors—such as the amount and number of all drugs abused; extent of prenatal care; possible neglect or abuse of the child; exposure to violence in the environment; socioeconomic conditions; maternal nutrition; other health conditions; and exposure to sexually-transmitted diseases—can contribute to the difficulty in determining direct impact of prenatal cocaine use on maternal, fetal, and child outcomes.
Many recall that “crack babies,” or babies born to mothers who used crack cocaine while pregnant, were at one time written off by many as a lost generation. They were predicted to suffer from severe, irreversible damage, including reduced intelligence and social skills. It was later found that this was a gross exaggeration. However, the fact that most of these children appear normal should not be overinterpreted as indicating that there is no cause for concern. Using sophisticated technologies, scientists are now finding that exposure to cocaine during fetal development may lead to subtle, yet significant, later deficits in some children, including deficits in some aspects of cognitive performance, information-processing, and attention to tasks—abilities that are important for success in school.
There was an enormous increase in the number of people seeking treatment for cocaine addiction during the 1980s and 1990s. Treatment providers in most areas of the country, except in the West and Southwest, report that cocaine is the most commonly cited drug of abuse among their clients. The majority of individuals seeking treatment smoke crack, and are likely to be polydrug users, or users of more than one substance. The widespread abuse of cocaine has stimulated extensive efforts to develop treatment programs for this type of drug abuse. Cocaine abuse and addiction is a complex problem involving biological changes in the brain as well as a myriad of social, familial, and environmental factors. Therefore, treatment of cocaine addiction is complex, and must address a variety of problems. Like any good treatment plan, cocaine treatment strategies need to assess the psychobiological, social, and pharmacological aspects of the patient’s drug abuse.

Pharmacological Approaches
There are no medications currently available to treat cocaine addiction specifically. Consequently, NIDA is aggressively pursuing the identification and testing of new cocaine treatment medications. Several newly emerging compounds are being investigated to assess their safety and efficacy in treating cocaine addiction.Topiramate and modafanil, two marketed medications, have shown promising signals as potential cocaine treatment agents. Additionally, baclofen, a GABA-B agonist, showed promise in a subgroup of cocaine addicts with heavy use patterns. Because of mood changes experienced during the early stages of cocaine abstinence, antidepressant drugs have been shown to be of some benefit. In addition to the problems of treating addiction, cocaine overdose results in many deaths every year, and medical treatments are being developed to deal with the acute emergencies resulting from excessive cocaine abuse.
Behavioral Interventions
Many behavioral treatments have been found to be effective for cocaine addiction, including both residential and outpatient approaches. Indeed, behavioral therapies are often the only available, effective treatment approaches to many drug problems, including cocaine addiction, for which there is, as yet, no viable medication. However, integration of both types of treatments may ultimately prove to be the most effective approach for treating addiction. Disulfiram (a medication that has been used to treat alcoholism), in combination with behavioral treatment, has been shown, in clinical studies, to be effective in reducing cocaine abuse. It is important that patients receive services that match all of their treatment needs. For example, if a patient is un-employed, it may be helpful to provide vocational rehabilitation or career counseling. Similarly, if a patient has marital problems, it may be important to offer couples counseling. A behavioral therapy component that is showing positive results in many cocaine-addicted populations is contingency management. Contingency management may be particularly useful for helping patients achieve initial abstinence from cocaine. Some contingency management programs use a voucher-based system to give positive rewards for staying in treatment and remaining cocaine free. Based on drug-free urine tests, the patients earn points, which can be exchanged for items that encourage healthy living, such as joining a gym, or going to a movie and dinner.
Cognitive-behavioral therapy, or “Relapse Prevention,” is another approach. Cognitive-behavioral treatment, for example, is a focused approach to helping cocaine-addicted individuals abstain—and remain abstinent—from cocaine and other substances. The underlying assumption is that learning processes play an important role in the development and continuation of cocaine abuse and dependence. The same learning processes can be employed to help individuals reduce drug use and successfully cope with relapse. This approach attempts to help patients recognize, avoid, and cope; i.e., recognize the situations in which they are most likely to use cocaine, avoid these situations when appropriate, and cope more effectively with a range of problems and problematic behaviors associated with drug abuse. This therapy is also noteworthy because of its compatibility with a range of other treatments patients may receive, such as pharmacotherapy.
Therapeutic communities (TCs), or residential programs with planned lengths of stay of 6 to 12 months, offer another alternative to those in need of treatment for cocaine addiction. TCs focus on resocialization of the individual to society, and can include on-site vocational rehabilitation and other supportive services. Of course, there is variation in the types of therapeutic processes offered in TCs.
Addiction: A chronic, relapsing disease, characterized by compulsive drug-seeking and use and by neurochemical and molecular changes in the brain.
Anesthetic: An agent that causes insensitivity to pain.
Antidepressants: A group of drugs used in treating depressive disorders.
Cocaethylene: Potent stimulant created when cocaine and alcohol are used together.
Coca: The plant, Erythroxylon, from which cocaine is derived. Also refers to the leaves of this plant.
Crack: "Slang" term for a smokable form of cocaine.
Craving: A powerful, often uncontrollable desire for drugs.
Dopamine: A neurotransmitter present in regions of the brain that regulate movement, emotion, motivation, and the feeling of pleasure.
Neuron: A nerve cell in the brain.
Physical dependence: An adaptive physiological state that occurs with regular drug use and results in a withdrawal syndrome when drug use is stopped; usually occurs with tolerance.
Polydrug user: An individual who uses more than one drug.
Rush: A surge of pleasure that rapidly follows administration of some drugs.
Tolerance: A condition in which higher doses of a drug are required to produce the same effect as during initial use; often is associated with physical dependence.
Vertigo: The sensation of dizziness.
Withdrawal: A variety of symptoms that occur after use of an addictive drug is reduced or stopped
Gold, Mark S. Cocaine (and Crack): Clinical Aspects (181–198), Substance Abuse: A Comprehensive Textbook, Third Edition, Lowinson, ed. Baltimore, MD: Williams & Wilkins, 1997.
Harvey, John A. and Kosofsky, Barry, eds. Cocaine: Effects on the Developing Brain. Annals of the New York Academy of Sciences, Volume 846, 1998.
National Institute on Drug Abuse. Epidemiologic Trends in Drug Abuse: Advance Report, Community Epidemiology Work Group. NIH Pub. No. 03-5363A. Washington, DC: Supt. of Docs., U.S. Govt. Print. Off., June 2003.
National Institute on Drug Abuse. NIDA InfoFacts, Crack and Cocaine, 1998.
National Institute on Drug Abuse. National Survey Results on Drug Use From the Monitoring the Future Survey, 2003.
Office of National Drug Control Policy. The National Drug Control Strategy, 1998: A Ten Year Plan.
Shoptaw, S. et al. Randomized placebo-controlled trial of baclofen for cocaine dependence: preliminary effects for individuals with chronic patterns of cocaine use. J. Clin. Psychiatry, 64(12):1440–1448, 2003.
Snyder, Solomon H. Drugs and the Brain (122–130). New York: Scientific American Library, 1996.
Substance Abuse and Mental Health Services Administration. National Survey on Drug Use and Health. SAMHSA, 2002.


